What is immunosenescence?
Immunosenescence is the age-related decline and remodeling of the immune system. It involves thymic shrinkage (thymic involution), accumulation of senescent immune cells, and chronic low-grade inflammation known as inflammaging. These changes lead to poorer vaccine responses, increased infection risk, and higher susceptibility to autoimmune conditions and cancer in older adults.
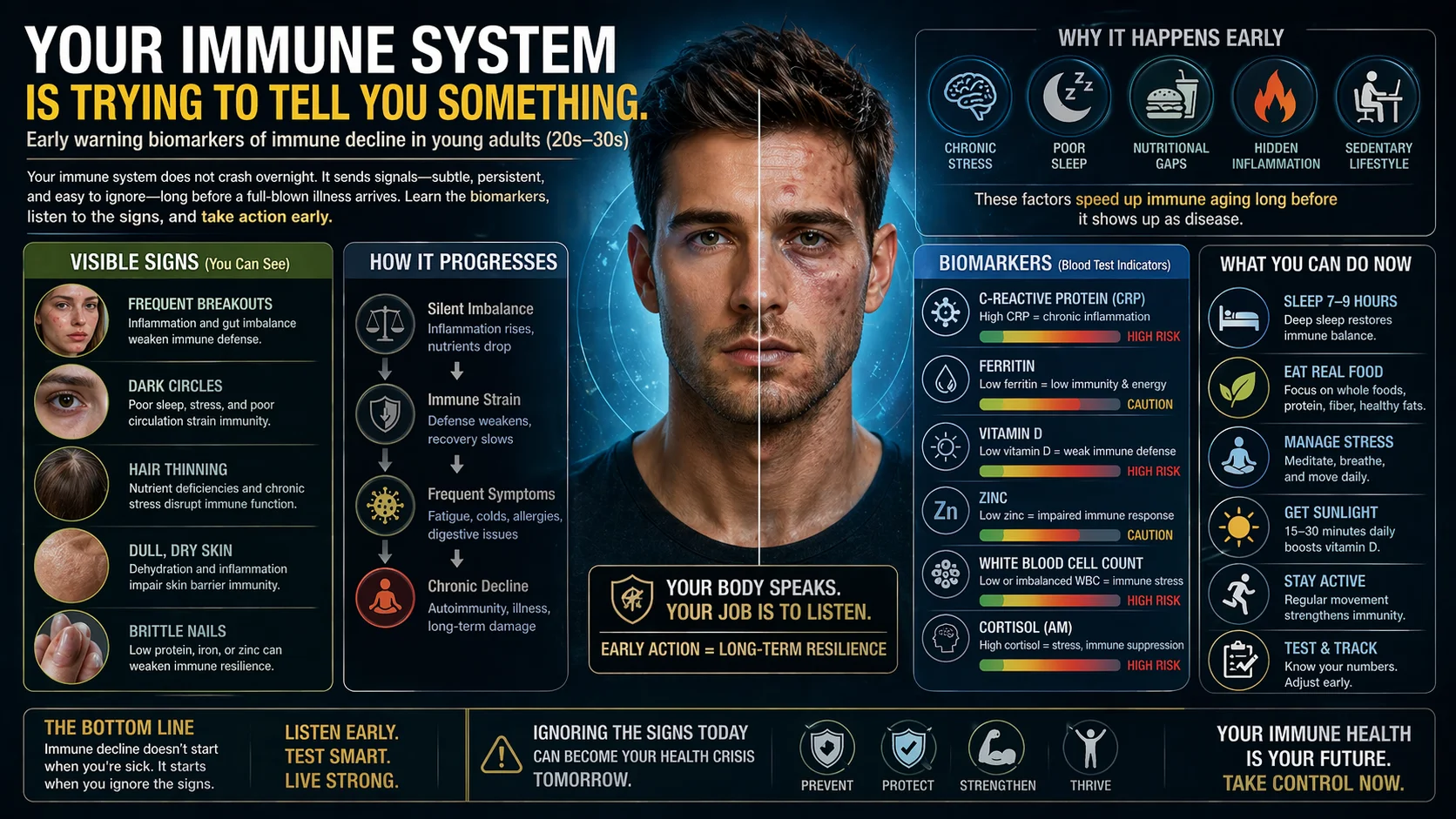
Your immune system does not crash overnight. It sends signals—subtle, persistent, and easy to ignore—long before a full-blown illness arrives.
Most young adults believe that being in their 20s or 30s grants them immunity from immune decline. After all, youth is supposed to be the peak of health, right? The truth is more complicated. Immune function follows a predictable trajectory, but lifestyle factors—chronic stress, poor sleep, nutritional gaps, and hidden inflammation—can accelerate decline years or even decades before it becomes obvious.
Understanding the early warning biomarkers of immune decline in young adults is not about becoming paranoid about your health. It is about learning to read your body’s language so you can intervene early, reverse damage, and build resilience before a crisis forces your attention.
This article outlines the most scientifically validated biomarkers—measurable signs—that your immune system is struggling. Some you can see. Some you can feel. Some require a simple blood test. All of them matter.

What Are Biomarkers? Why They Matter for Immune Health
A biomarker (biological marker) is a measurable indicator of a biological state or condition. Think of biomarkers as your body’s dashboard warning lights. Just as your car’s check engine light signals a problem before the engine fails, immune biomarkers signal trouble before you develop frequent infections, autoimmune conditions, or chronic fatigue.
For young adults, early detection is especially valuable because the immune system is highly adaptable. Interventions that work in your 20s and 30s—improving sleep, reducing stress, correcting nutrient deficiencies—can restore immune function more effectively than the same interventions attempted a decade later.
Here are the most important early warning biomarkers of immune decline in young adults, organized from the most scientifically validated to the most emerging.
1. Low Vitamin D Levels (Below 30 ng/mL)
What it measures: Serum 25-hydroxyvitamin D concentration
Why it matters: Vitamin D is not just a vitamin—it is a critical immune modulator. Your immune cells have vitamin D receptors, and without adequate vitamin D, these cells cannot function properly. Low vitamin D is consistently associated with increased risk of respiratory infections, autoimmune diseases, and poor vaccine responses.
The threshold: Optimal immune function requires levels between 40–60 ng/mL. Levels below 30 ng/mL are considered deficient and represent a clear early warning biomarker.
What young adults need to know: Vitamin D deficiency is epidemic among young adults, especially those who work indoors, live in northern latitudes, or consistently use sunscreen. One study found that over 40% of young adults have suboptimal vitamin D levels.
Action step: Request a blood test for 25-hydroxyvitamin D. If low, supplement with 1,000–4,000 IU daily, preferably with vitamin K2 and a fat-containing meal for absorption.
2. High-Sensitivity C-Reactive Protein (hs-CRP) Above 2 mg/L
What it measures: Low-grade systemic inflammation
Why it matters: C-reactive protein (CRP) is produced by your liver in response to inflammation. Standard CRP tests detect major inflammation (like from an infection or injury). The high-sensitivity version (hs-CRP) detects subtle, chronic inflammation that you cannot feel but that slowly degrades immune function over time.
The threshold:
- Low risk: hs-CRP below 1 mg/L
- Average risk: 1–3 mg/L
- High risk (warning zone): Above 3 mg/L
What young adults need to know: A persistently elevated hs-CRP in an otherwise healthy young adult is one of the most important early warning biomarkers of immune decline in young adults. It suggests your immune system is stuck in a chronic “on” state—constantly fighting something that isn’t there. This leads to immune exhaustion, where your body becomes less able to respond to real threats.
Common causes in young adults: Poor diet (high sugar, refined carbs, seed oils), chronic stress, poor sleep, hidden infections (gum disease, gut dysbiosis), and obesity.
Action step: Request hs-CRP (not standard CRP) from your doctor. If elevated, focus on anti-inflammatory lifestyle changes: Mediterranean diet, 7–9 hours of sleep, daily movement, and stress reduction.
3. Low Lymphocyte Count (Below 1.5 x 10⁹/L)
What it measures: Absolute lymphocyte count (part of a complete blood count or CBC)
Why it matters: Lymphocytes (B cells, T cells, and natural killer cells) are the master strategists of your immune system. They remember past infections, coordinate attacks, and destroy infected or cancerous cells. A persistently low lymphocyte count—called lymphopenia—is a direct sign of immune suppression.
The threshold: Normal range is typically 1.5–4.0 x 10⁹/L. Values consistently below 1.5 represent a warning. Values below 0.8 are clinically significant.
What young adults need to know: Mild lymphopenia is surprisingly common in young adults with high stress, poor sleep, or recent viral infections. However, if your lymphocyte count stays low for months without explanation, it warrants further investigation.
Action step: Review your complete blood count (CBC). If lymphocytes are low, prioritize sleep (lymphocytes regenerate during deep sleep), reduce alcohol, and check for nutrient deficiencies (zinc, selenium, vitamin A).
4. Elevated Neutrophil-to-Lymphocyte Ratio (NLR) Above 2.5
What it measures: The ratio of neutrophils (first-responder immune cells) to lymphocytes (adaptive immune cells)
Why it matters: The NLR is a powerful and underutilized biomarker of immune balance. A high NLR indicates that your body is in a chronic “fight” mode (high neutrophils) at the expense of long-term immune memory (low lymphocytes). Elevated NLR has been linked to increased infection risk, poor vaccine responses, and even higher mortality from all causes.
The threshold:
- Optimal: Below 1.5
- Normal: 1.5–2.5
- Warning zone: Above 2.5
- High risk: Above 3.5
What young adults need to know: NLR can be calculated for free from any standard CBC (divide absolute neutrophil count by absolute lymphocyte count). It costs nothing but is rarely discussed. Young adults with chronic stress, poor sleep, or hidden inflammation often have NLRs above 3.0 without knowing it.
Action step: Calculate your NLR from your last CBC. If above 2.5, address the root causes: stress management, sleep hygiene, and anti-inflammatory nutrition.
5. Low Natural Killer (NK) Cell Activity
What it measures: How effectively your natural killer cells destroy infected or cancerous cells
Why it matters: NK cells are your immune system’s rapid-response special forces. They do not need prior exposure to a threat—they simply recognize and destroy cells that look abnormal. Low NK cell activity is one of the most direct early warning biomarkers of immune decline in young adults, predicting increased risk of viral infections (including severe COVID-19, herpes outbreaks, and HPV persistence) and even certain cancers.
The threshold: Measured via functional assay (not a standard blood test). Results vary by lab, but generally, activity below 10% lysis (destruction of target cells) is concerning.
What young adults need to know: This test is not routine. It requires a specialized blood draw and is typically ordered only when immune deficiency is suspected. However, if you suffer from recurrent viral infections (cold sores, shingles, warts, frequent colds), requesting NK cell activity testing can provide invaluable information.
Action step: Ask an immunologist or functional medicine doctor for an NK cell activity panel. Interventions that boost NK activity include beta-glucans (from medicinal mushrooms like reishi and turkey tail), moderate exercise, and adequate sleep.
6. Low Serum Zinc (Below 80 mcg/dL)
What it measures: Zinc concentration in your blood
Why it matters: Zinc is essential for the development and function of immune cells, including neutrophils, natural killer cells, and T-cells. Even mild zinc deficiency impairs your ability to fight infections. Zinc also acts as an antioxidant, protecting immune cells from damage.
The threshold:
- Deficient: Below 60 mcg/dL
- Marginal (warning zone): 60–80 mcg/dL
- Optimal: 80–120 mcg/dL
What young adults need to know: Zinc deficiency is common in young adults who eat vegetarian or vegan diets (plant-based zinc is poorly absorbed), have digestive issues, or take certain medications (including some antacids and diuretics). Marginal deficiency often causes no obvious symptoms but silently suppresses immune function.
Action step: Request serum zinc testing. If low or marginal, increase dietary zinc (oysters, beef, pumpkin seeds, chickpeas) or supplement with 15–30 mg of chelated zinc (zinc picolinate or zinc bisglycinate) with food.
7. Poor Sleep Quality (Objectively Measured)
What it measures: Sleep duration, efficiency, and consistency (measured via actigraphy or sleep diary)
Why it matters: Sleep is not rest—it is active immune maintenance. During deep sleep, your body releases cytokines that coordinate immune responses, produces memory T-cells, and clears inflammatory debris from the brain. Chronic poor sleep is now recognized as one of the most powerful predictors of immune decline.
The threshold: Less than 7 hours of sleep per night, frequent nighttime awakenings, or inconsistent sleep-wake timing (social jet lag) all qualify as warning signs.
What young adults need to know: You cannot out-supplement poor sleep. No vitamin, no herb, no superfood compensates for chronic sleep deprivation. If you consistently sleep less than 7 hours or wake up unrefreshed, this is arguably the most important early warning biomarker of immune decline in young adults because it drives nearly all others (elevated inflammation, low lymphocytes, high NLR).
Action step: Track your sleep for two weeks. Prioritize 7–9 hours nightly. If you cannot achieve this despite effort, consult a sleep specialist. Do not accept chronic poor sleep as normal—it is not.
How to Monitor Your Immune Biomarkers: A Practical Guide
You do not need to test everything at once. Here is a sensible, step-by-step approach:
Year 1 (Baseline)
| Test | Frequency | Approximate Cost (US, without insurance) |
|---|---|---|
| Complete Blood Count (CBC) with differential | Annually | $15–30 |
| High-sensitivity CRP (hs-CRP) | Annually | $10–20 |
| Vitamin D (25-hydroxy) | Annually | $40–60 |
| Serum zinc | Annually | $20–40 |
If Any Baseline Marker Is Abnormal
- Repeat testing in 3–6 months after lifestyle interventions
- Add more specialized tests (NLR calculation from CBC is free; NK cell activity only if clinically indicated)
Free Daily Biomarkers You Can Track Right Now
- Sleep quality (duration, how you feel upon waking)
- Recovery from minor illnesses (colds resolve within 7–10 days? or linger for weeks?)
- Wound healing speed (small cuts heal within days? or become infected?)
- Digestive regularity (chronic bloating or irregularity suggests gut-immune disruption)
- Energy stability (consistent energy throughout the day? or afternoon crashes?)
What to Do If Your Biomarkers Show Decline
Finding that one or more of your biomarkers fall into the warning zone is not a reason for panic. It is a reason for action. The young adult immune system is remarkably plastic—it can recover quickly when given the right conditions.
The 4-Pillar Immune Restoration Protocol
| Pillar | Action Steps | Expected Timeline for Improvement |
|---|---|---|
| Sleep | 7–9 hours nightly; consistent bedtime/wake time (even weekends); no screens 60 minutes before bed | hs-CRP and NLR improve within 2–4 weeks |
| Nutrition | Anti-inflammatory diet (vegetables, fruits, fatty fish, olive oil); correct zinc and vitamin D deficiencies | Vitamin D and zinc normalize within 2–3 months of supplementation |
| Stress | Daily stress management (meditation, breathwork, nature exposure); reduce caffeine and alcohol | Lymphocyte count can rise within 1–2 months of cortisol reduction |
| Movement | Moderate exercise (30–45 minutes, 5 days/week) – not overtraining (which suppresses immunity) | NK cell activity improves within weeks of regular moderate exercise |
When to See a Doctor
Consult an immunologist or functional medicine physician if:
- Multiple biomarkers are abnormal despite 3–6 months of lifestyle intervention
- You experience recurrent, severe, or unusual infections (pneumonia twice in one year, shingles under age 40, persistent fungal infections)
- You have unexplained fevers, night sweats, or unintended weight loss alongside abnormal biomarkers
Conclusion: Your Biomarkers Are Talking. Are You Listening?
The early warning biomarkers of immune decline in young adults are not hidden in expensive, experimental tests. Most are available through standard blood work that costs less than a dinner out. A complete blood count, vitamin D level, hs-CRP, and serum zinc—plus an honest assessment of your sleep—will tell you more about your immune trajectory than any symptom checklist ever could.
The mistake young adults make is assuming that “feeling fine” means everything is fine. But immune decline is silent. It does not announce itself with dramatic symptoms. It whispers through slightly elevated inflammation, slightly low lymphocytes, slightly poor sleep. And if you ignore those whispers long enough, they become shouts—autoimmune disease, chronic fatigue, cancer, or simply being the person who catches every cold that passes through the office.
You have the power to listen now. Test your biomarkers. Interpret them honestly. Take action. Your future immune self will thank you.
Frequently Asked Questions
Can immune decline be reversed in young adults?
Yes, largely. Unlike older adults whose immune systems naturally decline with age (immunosenescence), young adults typically experience functional decline driven by lifestyle factors. Correcting sleep, nutrition, stress, and nutrient deficiencies can restore immune function within weeks to months.
How often should young adults test immune biomarkers?
Annually for baseline markers (CBC, hs-CRP, vitamin D, zinc). If abnormal, repeat every 3–6 months until normalized. If normal and lifestyle is healthy, every 1–2 years is sufficient.
Are there any reliable at-home tests for immune biomarkers?
Yes, several companies offer at-home finger-prick tests for vitamin D, hs-CRP, and some inflammatory markers. However, CBC (which provides lymphocytes, neutrophils, and NLR) typically requires a venous blood draw. Use at-home tests as screening tools, not diagnostic replacements.
Do vaccines affect these biomarkers?
Temporarily, yes. Vaccination triggers an immune response that can elevate hs-CRP and alter lymphocyte counts for days to weeks. Avoid testing within 2–4 weeks of any vaccination for accurate baseline results.
What is the single most important biomarker for young adults?
If you can only test one thing, test vitamin D. It is inexpensive, deficiency is epidemic, and correction has profound immune benefits. If you can test two, add hs-CRP to assess hidden inflammation.
Medical Disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before ordering tests, interpreting results, or making significant lifestyle or supplement changes.






